Autism Spectrum Disorder
Autism Spectrum Disorder
What is it?
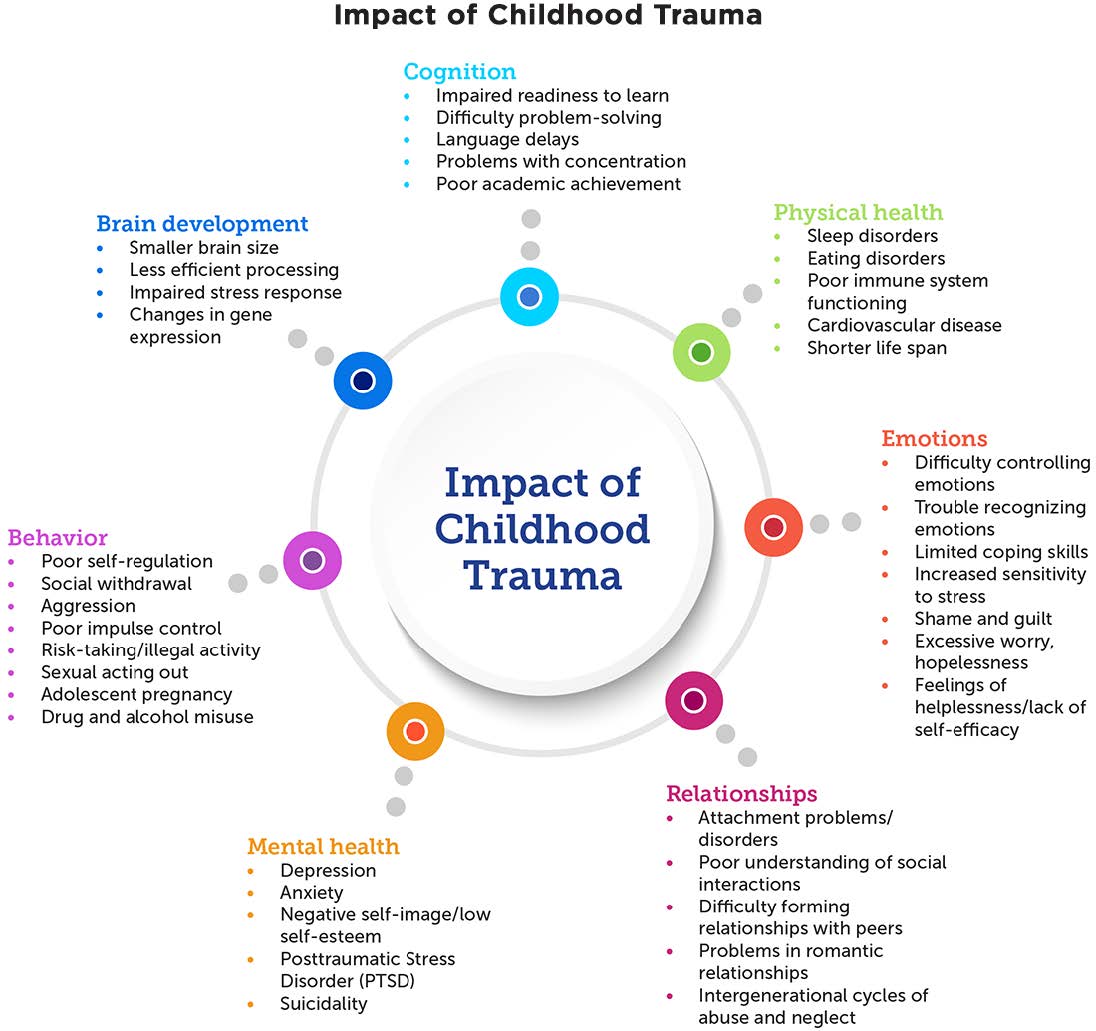
Autism spectrum disorder (ASD) refers to a group of neurodevelopmental disorders that affect how people communicate, learn, behave, and socially interact.
What are common signs of ASD?
Children and youth with ASD usually experience two types of symptoms:
- Social impairment and communication difficulties
- Avoids or does not keep eye contact
- Does not respond to name
- Does not show facial expressions like happy, sad, angry, and surprised
- Does not play simple interactive games
- Uses few or no gestures (e.g. does not point at what you point to or wave goodbye)
- Does not share interests with others
- Does not notice when others are hurt or sad
- Does not pretend in play
- Shows little interest in peers
- Has trouble understanding other people’s feelings or talking about own feelings
- Does not play games with turn-taking
- Repetitive or restricted behaviours
- Lines up toys or other objects and gets upset when order is changed
- Repeats the same words or phrases over and over
- Plays with toys the same way every time
- Is focused on parts of objects
- Has obsessive interests
- Must follow certain routines and gets upset by minor changes
- Flaps hands or rocks body in circles
- Has unusual reactions to the way things sound, smell, taste, look or feel
- More sensitive or less sensitive than others to sensory experiences (pain, temperature, texture, smell, taste, or sound)
Other signs:
- Delayed language skills
- Delayed movement skills
- Delayed cognitive or learning skills
- Hyperactive, impulsive, and/or inattentive behaviour
- Epilepsy or seizure disorder
- Unusual eating and sleeping habits
- Gastrointestinal issues
- Unusual mood or emotional reactions
- Anxiety
- Lack of fear or more fear than expected
- Self-harm
When is it time to seek professional help?
ASD symptoms can vary greatly from child to child depending on the severity of the disorder. Children should be screened for developmental delays during periodic checkups.
You may also want to consider these tools:
What makes ASD difficult to diagnose in children?
- Symptoms of one disorder can look like another disorder.
- Symptoms of one disorder can hide symptoms of another disorder.
- Symptoms can vary greatly from child to child.
- There are only a few guidelines and tests that help to diagnose other mental challenges in children with ASD.
What can be done?
Educational/behavioural interventions
Early behavioural/educational interventions have been very successful in many children with ASD. In these interventions, highly structured and intensive skill-oriented training sessions are used to help children develop social and language skills.
Applied Behavioural Analysis (ABA) is a type of therapy that can improve social, communication, and learning skills through reinforcement strategies.
Modified Cognitive Behavioural Therapy (CBT) is an example of behavioural intervention. Cognitive Behavioural Therapy (CBT) teaches people to examine and change the way they think (cognitive), act (behaviour) and feel (emotionally and physically). Cognitive Behavior Therapy (CBT) is beneficial to people with Autism Spectrum Disorder (ASD) but scientists suggest that the method needs to be modified in relation to the child’s cognitive profile.
Medications
While there is no medication that can treat ASD itself or even its main symptoms, there are medications that can help with related symptoms such as anxiety, depression, schizophrenia and obsessive-compulsive disorder. Antipsychotic medications are used to treat severe behavioural problems. Seizures can be treated with one or more anticonvulsant drugs. Medication used to treat people with attention deficit disorder can be used effectively to help decrease impulsivity and hyperactivity in people with ASD.
What makes some children more vulnerable to ASD?
Scientists believe that both genetics and environment likely play a role in ASD. ASD is a complex disorder that is the result of many interacting genes as well as the result of genes interacting with the environment.
Autism is more common in children born prematurely. Studies suggest that ASD could be a result of disruptions in brain growth very early in the child’s brain development. These disruptions may be the result of weakness in genes that control brain development and regulate how brain cells communicate with each other.
Where can I access support?
An early diagnosis is important so that the child can get the help they need. Talk to the child’s family doctor or pediatrician. The doctor can refer the child to the BC Autism Assessment Network (BCCAAN) for further assessment and diagnosis.
Contact Autism Information Services BC (AIS BC), a provincial information centre for autism and related disorders. AIS BC has information on assessment, diagnosis and treatment options, and you can reach them by phone, in person or via email.
Talk to the child’s guardianship worker to explore what options are available for assessment so their diagnosis and treatment plan can be included in their Care Plan. The guardianship worker will help make appropriate referrals for specialized supports and services.
Phone
Main:
604-544-1110
Toll-Free Foster Parent Line:
1-800-663-9999
Office hours: 8:30 am - 4:00 pm, Monday to Friday
PROVINCIAL CENTRALIZED SCREENING
Foster parents are encouraged to call this number in the event of an EMERGENCY or CRISIS occurring after regular office hours:
1-800-663-9122
REPORT CHILD ABUSE
If you think a child or youth under 19 years of age is being abused or neglected, you have the legal duty to report your concern to a child welfare worker. Phone 1-800-663-9122 at any time of the day or night. Visit the Government of BC website for more info.
address
BCFPA Provincial Office
Suite 208 - 20641 Logan Avenue
Langley, BC V3A 7R3
contact us
Fill out our contact form...

News
Site menu
Subscribe to Our Newsletter
Charitable Registration #
106778079 RR 0001
Our work takes place on the traditional and unceded Coast Salish territories of the Kwantlen, Katzie, Matsqui and Semiahmoo First Nations. BCFPA is committed to reconciliation with all Indigenous communities, and creating a space where we listen, learn and grow together.
© 2021 BC Foster Parents. Site design by Mighty Sparrow Design.